Blog

A Meaningful Collaboration Between Rutgers Business School and Delphine Diagnostics Inc
A Meaningful Collaboration Between Rutgers Business School and Delphine Diagnostics Inc In the pictures: Delphine’s CEO, Andy (Andiappan) Bala, is working with the Rutgers Business

Healthcare companies discuss their interest in establishing themselves in Puerto Rico
Healthcare companies discuss their interest in establishing themselves in Puerto Rico We are so thrilled that Delphine Diagnostics’ leadership team participated in the Puerto Rico

Human Genomics and COVID-19
Human Genomics and COVID-19 The Human Genome is a beautiful and intricate system that encodes and inscribes the biological functions of our body. This multi-faceted blueprint is critical for not only creating and sustaining
Covid-19: Should we be worried about reports of myocarditis and pericarditis after mRNA vaccines?
Covid-19: Should we be worried about reports of myocarditis and pericarditis after mRNA vaccines? What is the latest? On 23 June the US Centers for
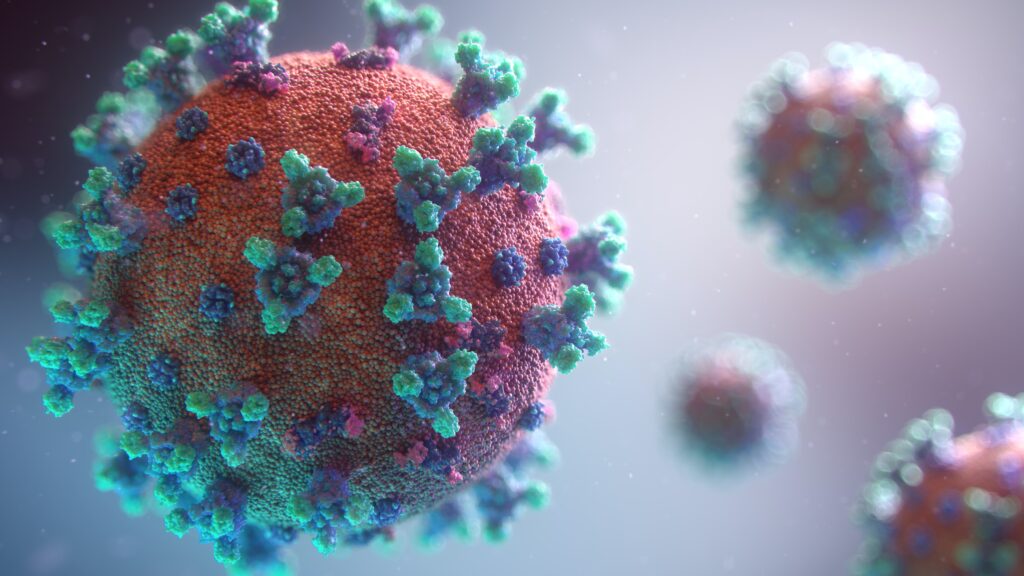
Delphine’s PrecisQT™ not affected by known SARS-CoV-2 VariantsCovid-19: Should we be worried about reports of myocarditis and pericarditis after mRNA vaccines?
A Perspective on the COVID-19 Vaccine Changes to the SARS-CoV-2 genome—including some of those found in currently circulating variants—can negatively affect the detection of the

Delphine Notification Accepted by FDA
Delphine Notification Accepted by FDA Delphine Diagnostics Inc., Bordentown, New Jersey, has been informed by the FDA’s Center for Devices and Radiological Health (CDRH) that
A Perspective on the COVID-19 Vaccine
A Perspective on the COVID-19 Vaccine For a country besieged for over a year by a virus that in addition to claiming over half a

